Medical Coding Automation Tools: How Healthcare Practices Are Improving Billing Efficiency

Healthcare providers across the United States are increasingly adopting
medical coding automation tools to improve billing accuracy, reduce administrative workload, and speed up insurance reimbursements.
As insurance requirements become more complex, manual coding processes can slow down claims submission and increase the risk of denials. Automated coding technology helps healthcare organizations streamline revenue cycle operations while maintaining compliance with payer guidelines.
In 2026, automation is becoming an important part of modern
medical billing and coding workflows, especially for practices handling high claim volumes.
This guide explains how
medical coding automation works, its benefits, limitations, and how healthcare providers can use automation effectively alongside experienced billing professionals.
What Are Medical Coding Automation Tools?
Medical coding automation tools use technologies such as:
- Artificial intelligence (AI)
- Natural language processing (NLP)
- Machine learning
- Revenue cycle automation software
These systems analyze clinical documentation and recommend appropriate:
- ICD-10 diagnosis codes
- CPT procedure codes
- HCPCS codes
The goal of automated medical coding is to reduce manual data entry and improve coding efficiency.
Instead of reviewing every patient chart manually, coders can use automation tools to identify coding suggestions faster and process claims more efficiently.
Why Healthcare Practices Are Adopting Medical Coding Automation
Healthcare providers are under constant pressure to improve operational efficiency while reducing claim denials.
Manual coding processes often create challenges such as:
- Coding inconsistencies
- Delayed claims submissions
- Administrative overload
- Human errors in documentation review
By implementing
medical coding automation software, practices can streamline repetitive tasks and improve workflow productivity.
According to industry reports, automation technologies can help reduce coding turnaround times and improve revenue cycle efficiency when combined with human oversight.
Benefits of Automated Medical Coding
Faster Claim Processing
One of the biggest advantages of automated medical coding tools is speed.
Automation helps coding teams process patient charts more efficiently, which allows claims to be submitted faster to insurance companies.
Faster submissions can improve reimbursement timelines and cash flow for healthcare practices.
Improved Coding Accuracy
AI-powered coding systems analyze clinical documentation and identify potential coding errors before claims are submitted.
This helps reduce:
- Incorrect CPT coding
- Missing diagnosis codes
- Documentation mismatches
- Claim rejections
Accurate coding is essential for reducing insurance denials and maintaining compliance with payer requirements.
Reduced Administrative Workload
Medical coders and billing teams often spend significant time reviewing repetitive documentation.
Automating the medical coding process allows staff to focus more on complex claims, denial management, and compliance monitoring. This can improve overall operational efficiency for healthcare organizations.
Better Revenue Cycle Management
Automation supports broader medical billing and coding automation strategies by improving claim tracking, coding consistency, and reporting.
Integrated revenue cycle management systems help practices monitor:
- Claim status
- Denial trends
- Coding performance
- Payment timelines
These insights help providers identify financial inefficiencies and optimize billing operations.
Limitations of Medical Coding Automation
Although automation technology continues to improve, it cannot fully replace experienced medical coders.
Complex cases still require human review, especially in specialties such as:
- Mental health billing
- Neurology
- Dermatology
- Surgical coding
AI systems may struggle with incomplete documentation or specialty-specific payer requirements.
That’s why many healthcare organizations use a
hybrid approach, combining automation tools with certified coding professionals.
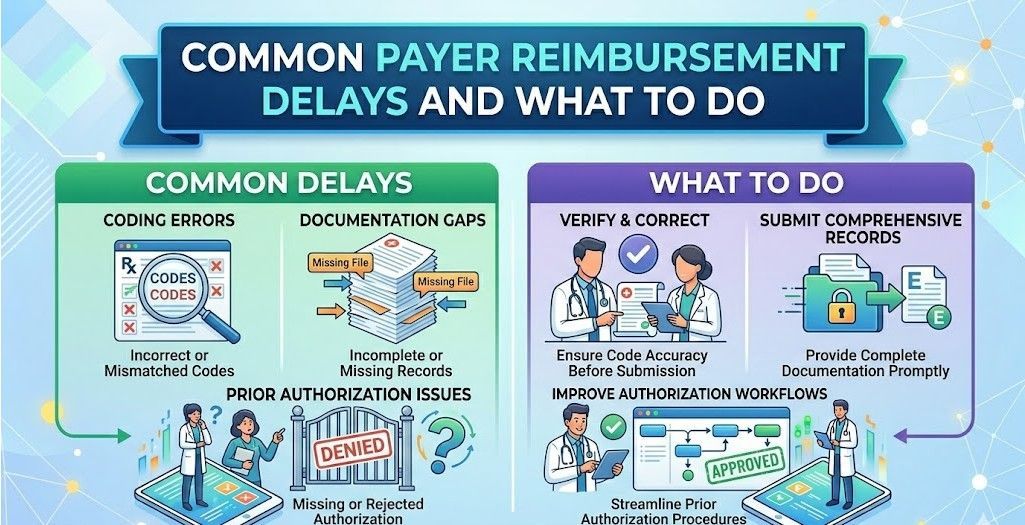
Also Read:
Common Payer Reimbursement Delays
Will Medical Coding Become Fully Automated?
One common question in the healthcare industry is: Will medical coding become automated?
While AI and automation are transforming healthcare billing, most experts believe human coders will continue to play an essential role.
Automation is designed to support coding teams, not completely replace them.
Human expertise is still required for:
- Compliance review
- Complex coding decisions
- Denial management
- Insurance audits
- Specialty billing requirements
The future of
AI medical coding automation will likely focus on improving efficiency while keeping certified coders involved in quality control and compliance oversight.
How Valley Medical Billing Uses Technology to Improve Billing Efficiency
At Valley Medical Billing, technology and human expertise work together to improve billing accuracy and reimbursement performance.
The company uses advanced billing workflows and coding support processes to help healthcare providers:
- Reduce claim denials
- Improve coding accuracy
- Streamline revenue cycle management
- Accelerate insurance reimbursements
By combining efficient billing systems with experienced professionals,
Valley Medical Billing helps healthcare practices maintain accurate and compliant medical billing operations.
FAQs
What is automated medical coding?
Automated medical coding uses AI and software tools to analyze clinical documentation and recommend ICD-10, CPT, and HCPCS codes for insurance billing.
Can AI replace medical coders?
No. AI can improve efficiency, but experienced coders are still necessary for compliance review, specialty coding, and complex claims management.
What are the benefits of medical coding automation tools?
Medical coding automation tools help improve coding speed, reduce administrative workload, minimize claim errors, and support better revenue cycle management.
Are automated medical coding tools accurate?
Modern coding automation tools can improve accuracy, but human review is still important to ensure proper coding and insurance compliance.